Women have made tremendous strides in the field of medicine over the past century. In spite of historical barriers and discrimination, women have contributed significantly to the medical field and made remarkable achievements. This blog post will highlight some of the most notable achievements of women in medicine as the Coding & Billing Solutions Team celebrates International Women’s Day 2024!
 Elizabeth Blackwell: The First Female Physician
Elizabeth Blackwell: The First Female Physician
Elizabeth Blackwell was the first woman to receive a medical degree in the United States. She earned her degree in 1849 from Geneva Medical College in New York, despite strong opposition from both faculty and students. Blackwell faced numerous challenges as a woman in a male-dominated field, including discrimination from medical institutions and difficulty securing clinical training opportunities. However, she persevered and went on to become a successful physician and a trailblazer for women in medicine.
In 1857, she co-founded the New York Infirmary for Indigent Women and Children, providing much-needed medical care to underserved populations while also creating opportunities for female physicians and nurses. Blackwell was also a strong advocate for public health reform and women’s medical education, helping to establish the London School of Medicine for Women in 1874. Her work paved the way for future generations of women in medicine, breaking barriers that had long excluded them from the profession.
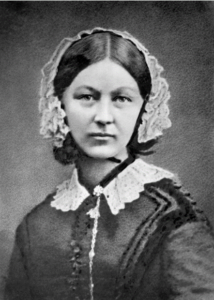 Florence Nightingale: The Founder of Modern Nursing
Florence Nightingale: The Founder of Modern Nursing
Florence Nightingale is widely regarded as the founder of modern nursing. Born in 1820 into a wealthy British family, she defied societal expectations by pursuing a career in healthcare, believing it to be her true calling. Nightingale gained international recognition during the Crimean War (1853–1856) for her groundbreaking work in improving the unsanitary conditions of military hospitals. Sent with a team of nurses to the British base hospital in Scutari, she was appalled by the filthy environment, lack of basic hygiene, and high mortality rates. Through rigorous sanitation practices, improved ventilation, and better nutrition, she dramatically reduced death rates from infections and preventable diseases, earning the nickname “The Lady with the Lamp” for her nightly rounds tending to wounded soldiers.
Beyond her wartime contributions, Nightingale was a visionary in public health and nursing education. In 1860, she established the Nightingale Training School for Nurses at St. Thomas’ Hospital in London, setting professional standards for nursing and emphasizing discipline, hygiene, and compassionate patient care. The school became a model for nursing education worldwide, influencing hospital practices in Europe, North America, and beyond.
Nightingale was also a pioneer in using statistical analysis to advocate for healthcare reform. She presented data in innovative ways, such as pie charts and diagrams, to illustrate the impact of sanitation on mortality rates. Her work laid the foundation for evidence-based nursing and public health policies.
Her influence extended far beyond her lifetime, shaping modern nursing as a respected and essential profession. Through her writings, including Notes on Nursing: What It Is and What It Is Not, she educated generations of nurses and health practitioners. Florence Nightingale’s legacy continues to inspire healthcare professionals worldwide, embodying the principles of dedication, innovation, and patient-centered care.
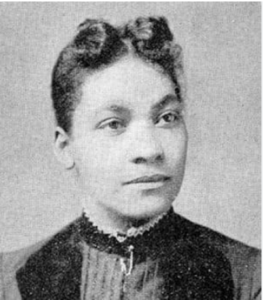 Dr. Rebecca Lee Crumpler: The First African American Female Physician
Dr. Rebecca Lee Crumpler: The First African American Female Physician
Dr. Rebecca Lee Crumpler was the first African American woman to receive a medical degree in the United States, breaking racial and gender barriers in the field of medicine. She earned her degree in 1864 from the New England Female Medical College in Boston, an institution dedicated to training women in medicine at a time when female physicians were rare. Dr. Crumpler’s admission and graduation were remarkable achievements, as the college awarded medical degrees to only a small number of women, and she was the first and only Black woman to earn her degree from the institution before it closed in 1873.
Throughout her career, Dr. Crumpler faced significant discrimination and prejudice, both as a woman and as an African American physician in a deeply segregated society. Despite these challenges, she remained dedicated to improving the health of her patients, particularly underserved communities. After the Civil War, she moved to Richmond, Virginia, to work with the Freedmen’s Bureau, providing medical care to formerly enslaved African Americans who had little access to healthcare. She treated patients who suffered from malnutrition, disease, and the lasting effects of enslavement, advocating for proper hygiene, nutrition, and preventive care.
Returning to Boston, Dr. Crumpler continued her medical work, primarily serving women and children in poor communities. She was deeply committed to public health and sought to educate her patients on disease prevention and overall well-being. In 1883, she published A Book of Medical Discourses, one of the first medical texts written by an African American. The book provided guidance on maternal and child health, reflecting her lifelong commitment to improving healthcare for women and children, especially those from disadvantaged backgrounds.
Dr. Crumpler’s pioneering efforts helped pave the way for future generations of Black women in medicine, inspiring change in a profession that had long excluded both women and people of color. Her resilience, dedication, and contributions to public health remain an essential part of American medical history.
 Dr. Virginia Apgar: Inventor of the Apgar Score
Dr. Virginia Apgar: Inventor of the Apgar Score
Dr. Virginia Apgar was a pioneering anesthesiologist, medical researcher, and the inventor of the Apgar Score, a revolutionary system used to assess the health of newborn babies immediately after birth. Born in 1909, she pursued a career in medicine at a time when women faced significant barriers in the field. She earned her medical degree from Columbia University’s College of Physicians and Surgeons in 1933 and initially trained as a surgeon. However, due to the limited opportunities for women in surgery, she shifted her focus to anesthesiology, becoming one of the first female physicians in the specialty. She later became the first woman to head a department at Columbia-Presbyterian Medical Center, leading the division of anesthesiology.
Dr. Apgar’s most significant contribution to medicine came in 1952 when she developed the Apgar Score, a quick and systematic way to evaluate newborns’ health in the critical minutes after birth. The score assesses five key criteria:
- Appearance (skin color)
- Pulse (heart rate)
- Grimace (reflex irritability)
- Activity (muscle tone)
- Respiration (breathing effort)
Each category is scored from 0 to 2, with a total possible score of 10. This simple yet effective method allows healthcare providers to determine whether a newborn requires immediate medical intervention. Before the Apgar Score, many cases of neonatal distress went unnoticed, leading to high infant mortality rates.
The Apgar Score was quickly adopted worldwide and remains a standard practice in obstetric and neonatal care. It has played a critical role in reducing infant mortality by helping doctors and nurses swiftly identify and address potential health issues in newborns.
Beyond her work in neonatal health, Dr. Apgar was also a passionate advocate for maternal and infant care. Later in her career, she worked for the March of Dimes, dedicating her efforts to birth defect prevention and public health education. She also earned a master’s degree in public health from Johns Hopkins University, broadening her impact in the medical community.
Dr. Apgar’s legacy extends beyond the score that bears her name—she inspired generations of women in medicine and helped transform the fields of anesthesiology, obstetrics, and neonatology. Her contributions continue to save countless lives and improve newborn care worldwide.
 Dr. Rosalind Franklin: Pioneering Researcher in DNA Structure
Dr. Rosalind Franklin: Pioneering Researcher in DNA Structure
Dr. Rosalind Franklin was a British chemist and X-ray crystallographer whose pioneering research played a crucial role in the discovery of the double-helix structure of DNA. Born in 1920 in London, Franklin excelled in science from an early age and earned a doctorate in physical chemistry from the University of Cambridge. She specialized in X-ray diffraction techniques, a method used to determine the atomic and molecular structure of crystals, which later became the foundation of her groundbreaking work on DNA.
In 1951, Franklin joined King’s College London, where she conducted research on the structure of deoxyribonucleic acid (DNA). Using X-ray diffraction, she captured high-resolution images of DNA fibers, including “Photograph 51”, which provided the clearest evidence that DNA had a helical structure. Her meticulous data analysis revealed critical insights into the molecule’s symmetry, density, and overall shape.
However, Franklin’s contributions were not fully recognized during her lifetime. Without her knowledge, Maurice Wilkins, a colleague at King’s College, showed “Photograph 51” to James Watson and Francis Crick at the University of Cambridge. This image and Franklin’s unpublished research notes became instrumental in helping Watson and Crick construct their famous DNA double-helix model in 1953. Though Watson, Crick, and Wilkins received the Nobel Prize in Physiology or Medicine in 1962, Franklin was not acknowledged, as the prize is not awarded posthumously.
Beyond DNA, Franklin made significant contributions to virology and coal chemistry. After leaving King’s College, she continued her research at Birkbeck College, where she studied the molecular structures of viruses, including the tobacco mosaic virus and polio virus, advancing the field of structural virology.
Dr. Rosalind Franklin passed away in 1958 at the age of 37 from ovarian cancer, possibly linked to prolonged exposure to X-ray radiation during her research. It was only in later years that her vital role in DNA’s discovery gained wider recognition, and she is now celebrated as a pioneer whose work laid the foundation for modern molecular biology. Today, numerous awards, research institutions, and scientific programs bear her name in honor of her lasting impact on science.
 Dr. Jane C. Wright: Pioneer of Chemotherapy
Dr. Jane C. Wright: Pioneer of Chemotherapy
Dr. Jane C. Wright was a trailblazing physician and researcher whose pioneering work in chemotherapy revolutionized cancer treatment. Born in 1919, she came from a distinguished medical family—her father, Dr. Louis T. Wright, was one of the first African American graduates of Harvard Medical School and a leader in medical research. Inspired by his legacy, she pursued a medical career and earned her M.D. from New York Medical College in 1945.
At a time when cancer treatment was largely limited to surgery and radiation, Dr. Wright conducted groundbreaking research on chemotherapy, helping to establish it as a viable treatment for cancer. In the 1940s and 1950s, chemotherapy was still experimental, and many doctors were skeptical of its potential. However, Dr. Wright’s innovative work at the Harlem Hospital Cancer Research Foundation, where she collaborated with her father, led to major advancements in the field. She studied the effects of various chemotherapy drugs on different types of cancer and developed new techniques for administering chemotherapy, including the use of catheters to deliver drugs directly into tumors, improving treatment precision and patient outcomes.
Throughout her career, Dr. Wright’s research contributed to the development of several effective chemotherapy agents, some of which remain foundational in cancer treatment today. Her studies helped expand the use of chemotherapy for patients with breast cancer, leukemia, lymphoma, and skin cancer.
In addition to her scientific contributions, Dr. Wright shattered racial and gender barriers in medicine. In 1971, she became the first woman elected president of the American Association for Cancer Research (AACR), a prestigious position that highlighted her influence in the oncology community. She was also a co-founder of the American Society of Clinical Oncology (ASCO) and served on the National Cancer Advisory Board, advising the U.S. government on cancer research and treatment strategies.
Dr. Wright was also a dedicated mentor and educator, serving as a professor of surgery and head of cancer chemotherapy research at New York Medical College, where she trained and inspired future generations of oncologists.
Her impact on chemotherapy and cancer treatment is immeasurable, and her pioneering efforts helped establish the field of medical oncology as we know it today. Dr. Wright’s legacy continues to inspire scientists and physicians, particularly women and African Americans in medicine, proving that innovation and perseverance can lead to life-saving advancements.
 Dr. Antonia Novello: First Female and Hispanic U.S. Surgeon General
Dr. Antonia Novello: First Female and Hispanic U.S. Surgeon General
Dr. Antonia Novello made history as the first female and first Hispanic Surgeon General of the United States, serving from 1990 to 1993 under President George H.W. Bush. A trailblazer in the medical and public health fields, Dr. Novello dedicated her career to addressing health disparities affecting underserved populations, particularly women, children, and minorities.
Born in 1944 in Puerto Rico, Novello overcame significant health challenges in her childhood, including a congenital intestinal condition that required multiple surgeries. Her experiences as a patient fueled her passion for medicine and a commitment to improving healthcare accessibility. She earned her M.D. from the University of Puerto Rico School of Medicine in 1970 and later specialized in pediatrics and nephrology. After further training at the University of Michigan and Johns Hopkins University, she joined the U.S. Public Health Service Commissioned Corps, where she focused on public health policy and advocacy.
As Surgeon General, Dr. Novello was a strong advocate for child health, launching initiatives to combat pediatric HIV/AIDS, childhood immunization gaps, and tobacco advertising targeted at young people. She played a key role in raising awareness of the dangers of smoking, particularly efforts to curb the marketing of cigarettes to children by tobacco companies.
She was also a champion for minority health, working to improve healthcare access for Hispanic and African American communities, and addressing issues like poor prenatal care, domestic violence, and the rising rates of underage drinking and drug use. Under her leadership, the Office of Minority Health expanded its efforts to bridge healthcare disparities and promote preventive medicine in marginalized communities.
Beyond her work in public health policy, Dr. Novello was a leading advocate for organ donation and transplantation, helping to increase awareness and promote organ donor programs nationwide. She emphasized the importance of educating the public about organ donation, particularly within communities of color, where donation rates were historically lower due to cultural misconceptions and lack of awareness.
After her tenure as Surgeon General, Dr. Novello continued her public health work, serving as the Commissioner of Health for the State of New York from 1999 to 2006, where she focused on issues such as obesity, mental health, and domestic violence. Her lifelong commitment to public service has earned her numerous awards, including recognition from the American Medical Association and the National Institutes of Health.
Dr. Novello’s groundbreaking achievements as a Latina woman in medicine paved the way for future generations of minority healthcare professionals and public health leaders. Her legacy continues to inspire efforts to make healthcare more equitable and accessible for all.
 Dr. Mae Jemison: First African American Woman in Space
Dr. Mae Jemison: First African American Woman in Space
Dr. Mae Jemison is a physician, engineer, and former NASA astronaut who made history in 1992 as the first African American woman to travel to space. Aboard the Space Shuttle Endeavour (STS-47), she conducted experiments on weightlessness, bone cell research, and human adaptation to space, contributing to advancements in space medicine. Before joining NASA, Jemison earned her M.D. from Cornell University and worked as a Peace Corps medical officer in West Africa, focusing on public health and disease prevention. Her diverse background in medicine, engineering, and international health made her a standout candidate when she was selected for NASA’s astronaut program in 1987.
Since leaving NASA, Dr. Jemison has been a leading advocate for STEM education and diversity in science and technology. She founded the Dorothy Jemison Foundation for Excellence, which runs programs like “The Earth We Share” to inspire young students in science. She also led the 100 Year Starship Project, an initiative exploring the feasibility of interstellar travel. As a sought-after speaker, she encourages greater inclusion in STEM fields, emphasizing that space exploration and scientific advancements must be accessible to all. Jemison’s pioneering career continues to inspire future generations of scientists, engineers, and astronauts to break barriers and reach for the stars.
 Dr. Jennifer Doudna & Dr. Emmanuelle Charpentier : The “Mother’s” of CRISPR”
Dr. Jennifer Doudna & Dr. Emmanuelle Charpentier : The “Mother’s” of CRISPR”
While there are many other scientists around the world that have contributed to the discovery of the CRISPR-Cas system, two scientists were the very first researchers who were instrumental in the discovery and adoption of CRISPR as a genome editing tool.
Dr. Jennifer Doudna:
Jennifer Doudna is the biggest household name in the world of CRISPR, and for good reason, she is credited as the one who co-invented CRISPR. Dr. Doudna was among the first scientists to propose that this microbial immunity mechanism could be harnessed for programmable genome editing. This tool has the potential to effectively change the genetic makeup of any organism and fix a near-infinite number of problems. Dr. Doudna’s discovery changed the world of genetic engineering as previous techniques were time-consuming, tedious, and nowhere as convenient as CRISPR.
Dr. Emmanuelle Charpentier
Emmanuelle Charpentier is the co-inventor of CRISPR. Together with Dr. Doudna, Dr. Charpentier was involved in the biochemical characterization of guide RNA and Cas9 enzyme-mediated DNA cleavage.
Her expertise in the fields of microbiology, biochemistry, and genetics helped pave the way for the discovery of CRISPR; work that was necessary for CRISPR to be discovered (as that discovery occurred working first with bacteria).
In 2020, Dr. Doudna and Dr. Charpentier received a Nobel prize in Chemistry for the discovery of CRISPR.
Women have made remarkable achievements in medicine throughout history, despite facing numerous challenges and barriers. From the first female physician to the first African American woman in space, these women have made significant contributions to the medical field and helped to improve the health and well-being of countless individuals. The accomplishments of these very special women in medicine serve as inspiration to us all.
Powered by Grey Matter Direct. Grey Matter Direct is a digital marketing agency in Mount Laurel, New Jersey, that specializes in website development, search engine optimization, email marketing, Google Ads and more.






 Elizabeth Blackwell: The First Female Physician
Elizabeth Blackwell: The First Female Physician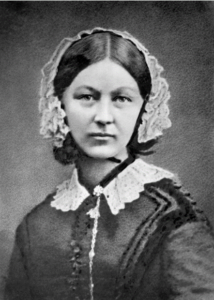 Florence Nightingale: The Founder of Modern Nursing
Florence Nightingale: The Founder of Modern Nursing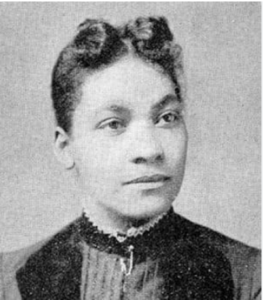 Dr. Rebecca Lee Crumpler: The First African American Female Physician
Dr. Rebecca Lee Crumpler: The First African American Female Physician Dr. Virginia Apgar: Inventor of the Apgar Score
Dr. Virginia Apgar: Inventor of the Apgar Score Dr. Rosalind Franklin: Pioneering Researcher in DNA Structure
Dr. Rosalind Franklin: Pioneering Researcher in DNA Structure Dr. Jane C. Wright: Pioneer of Chemotherapy
Dr. Jane C. Wright: Pioneer of Chemotherapy Dr. Antonia Novello: First Female and Hispanic U.S. Surgeon General
Dr. Antonia Novello: First Female and Hispanic U.S. Surgeon General Dr. Mae Jemison: First African American Woman in Space
Dr. Mae Jemison: First African American Woman in Space Dr. Jennifer Doudna & Dr. Emmanuelle Charpentier : The “Mother’s” of CRISPR”
Dr. Jennifer Doudna & Dr. Emmanuelle Charpentier : The “Mother’s” of CRISPR”


